Ask AAHA: Answers from the experts
When you have questions about your pet, you need expert answers quickly. AAHA Answers addresses some of your most common questions below. Your AAHA-accredited veterinary hospital can answer the rest!
Why AAHA?
-

Can I still take my pet to the vet during COVID-19?
Because of the important services veterinary hospitals provide in keeping pets healthy and safe as well as protecting public health, most veterinary practices will continue to provide as much of their regular services as possible during the COVID-19 pandemic. -

How can I prevent heatstroke in my pet?
After a long, cold winter, you’re likely ready to head outdoors for some fun in the sun. But, your adventure may be cut short if your pet develops heatstroke. Know common signs of heatstroke and take preventive measures to keep your pet cool through the dog days of summer. -

What Is Veterinary Physical Rehabilitation?
Pets can encounter many health challenges throughout their lives, from injuries and surgeries to age-related conditions, that impact their mobility and overall well-being. But all is not lost—the world of veterinary physical rehabilitation offers tailored solutions that will help your pet regain their strength, mobility, and quality of life. -

Should my pet get a massage?
The joys of a relaxing massage are no longer just for people. Pets also are reaping the benefits, as veterinary hospitals realize that the positive outcomes from a massage can go beyond calming and stress reduction to relieving pain and promoting optimal body function. -

How Can I Fix My Cat’s Behavior Problems?
Cats are mysterious creatures and understanding their behaviors can be a challenge. But, if your feline friend’s behaviors are frustrating, irksome, or downright dangerous, knowing the reason behind the action is key to effective management. Preserve the bond you share with your cat by learning to identify and manage common feline behavior problems. -

What is my pet's poop telling me?
We really do love our pets—enough that we will pick up their feces and even examine it for signs our furry companion is not feeling well. What seems like an insignificant pile of waste can tell you a lot about your pet’s overall health. -

Is my pet overweight?
Obesity is a growing trend that—unfortunately—is sweeping through many species, cats and dogs included. According to the Association for Pet Obesity Prevention surveys, the number of overweight pets has been growing as steadily as the number on the scale over the past decade. The most recent survey from 2022 classifies 59% of dogs and 61% of cats as overweight or obese, with one-third of pet owners believing their hefty pets are at an ideal weight. -

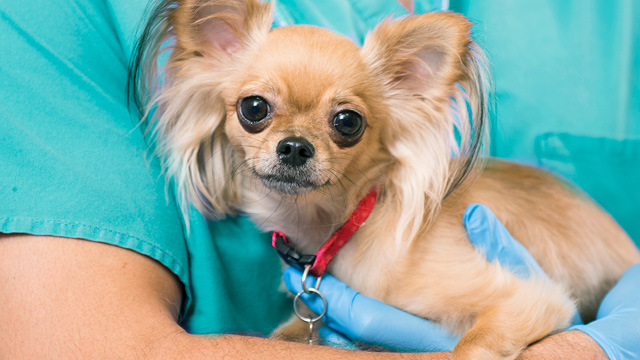
7 Steps for a Stress-Free Veterinary Visit
Have you ever skipped your pet’s veterinary visit because they don’t like going to the veterinarian? A veterinary hospital’s unfamiliar sights, sounds, and smells can cause some pets to become anxious. Unfortunately, pets don’t understand that poking them with needles, checking their temperature, touching their toes, or sticking instruments in their ears is beneficial to their health, and they can become stressed. In response to a stressful scenario, your pet’s brain enters fight-or-flight mode, and remembering previous visits can trigger repeated and worsening anxiety during future veterinary visits. -

What should I know about my puppy?
So, you just used the AAHA Canine Life Stage Calculator to determine that your dog is in the puppy stage of life. Congrats! Knowing your dog’s life stage helps you provide a lifetime of optimal care for your pooch. -

Is my dog at risk for cancer?
According to the National Cancer Institute , approximately 6 million new cancer diagnoses are made in dogs each year. Since not all pets receive medical care or a definitive cancer diagnosis, this number likely would rise if every pet saw a veterinarian annually. -

What should I know about my mature adult dog?
So, you just used the AAHA Canine Life Stage Calculator to determine that your dog is in the mature adult stage of life. Congrats! Knowing your dog’s life stage helps you provide a lifetime of optimal care. -

Can I take my dog camping?
Dogs enjoy romping in the great outdoors, and your canine companion would love to be included in your next camping trip. However, before packing your bags and hitting the trails, ensure you and your pooch are prepared for whatever nature has in store. -

When should I spay or neuter my pet?
As part of the battle against pet overpopulation, it used to be common practice to spay and neuter young pets as soon as it was safe to do so, and sterilization still is performed on shelter puppies and kittens. When it comes to privately-owned pets in secure homes, here are AAHA’s most recent recommendations. -

What should I know about my young adult dog?
So, you just used the AAHA Canine Life Stage Calculator to determine that your dog is in the young adult stage of life. Congr ats! Knowing your dog’s life stage helps you provide a lifetime of optimal care for your pooch. -

Why Won’t My Cat Use the Litter Box?
In addition to middle-of-the-night yowling for food, feline inappropriate elimination is a chief complaint of cat owners. When your cat fails to use the litter box appropriately, you likely become frustrated, which damages the bond you share with your feline friend. However, once you understand the reason behind your cat’s behavior, you can put effective solutions in place to resolve the issue and restore the relationship with your cat. -

How can I discourage my dog from running away?
Pets who run away can get lost, injured, or stolen. Although some dogs have a natural tendency to roam, there are many precautions you can take to prevent your furry friend from running away. -

Why does my pet shed?
While the amount of fur your pet sheds cannot be changed, the best way to prevent pet hair from accumulating in your home and on your clothes is to brush your pet daily. Ask your AAHA-accredited veterinarian to recommend a brush or comb that will work best for your pet’s coat, then get your pet used to regular brushing sessions. -

What is pancreatitis?
Pancreatitis is a painful inflammation of the pancreas that can make pets extremely ill. The pancreas is an abdominal organ located just below the stomach that produces digestive enzymes to break down dietary fats, proteins, and carbohydrates. The pancreas also produces insulin, which helps move glucose from the blood into cells for energy production. Pancreatitis can lead to dehydration, organ damage, diabetes, and insufficient enzyme production, and, in severe cases, can cause death.
-

Veterinary Telehealth
Does it take an act of Congress to get your cat in their carrier when it’s time to go to the veterinarian? Does your canine friend quake with fear when they face a veterinary visit? Veterinary telehealth may help relieve your furry friend’s stress and anxiety, as well as provide several other benefits. However, you should first learn the ins and outs of veterinary telehealth, so you know what to expect. -

Why Do Cats Knead?
Cat owners are likely familiar with their feline friend’s kneading behavior, or what many cat owners affectionately refer to as “making biscuits.” Similar to the way a baker pushes and pulls dough before baking, a kneading cat massages or repeatedly pushes their toes into a soft or cushioned surface, such as a plush blanket, fellow pet, or warm human lap. -

7 Steps for a Stress-Free Veterinary Visit
Have you ever skipped your pet’s veterinary visit because they don’t like going to the veterinarian? A veterinary hospital’s unfamiliar sights, sounds, and smells can cause some pets to become anxious. Unfortunately, pets don’t understand that poking them with needles, checking their temperature, touching their toes, or sticking instruments in their ears is beneficial to their health, and they can become stressed. In response to a stressful scenario, your pet’s brain enters fight-or-flight mode, and remembering previous visits can trigger repeated and worsening anxiety during future veterinary visits. -

Is a kidney transplant right for my pet?
Kidney failure is a leading cause of death in pet cats, with at least 30% of cats developing this devastating health condition as they age. Many treatment options exist, but they only manage clinical signs and slow disease progression, and are not a cure. -

Is a pocket pet right for me?
A furry little pet who loves to snuggle in your shirt pocket can be a great family addition. But, although rodents such as rats, mice, gerbils, and hamsters, as well as slightly larger guinea pigs, chinchillas, hedgehogs, and sugar gliders, may require less time and effort than a dog who expects daily walks, you should do your homework first. -

Why are regular veterinary visits important?
Visiting the veterinarian regularly is an important part of maintaining your pet’s health. Although your pet may look healthy, diseases often cause no obvious signs in their early stages. Wellness exams and screening tests allow your veterinary team to detect diseases before they progress and begin treatments that will extend your pet’s healthy years by your side. -

How can I safely walk my reactive dog?
You can walk your leash-reactive dog safely around your neighborhood, but she will need dedicated training and management. Many canines are sweet and happy pets at home, but when they step into unfamiliar territory with strange people and dogs, they bark, growl, snap, or quiver in fear, making a simple walk around the block into a scary, stressful situation. -

What is a veterinary technician?
Veterinary technicians are educated professionals who help veterinarians care for pets by providing nursing support, acting as patient advocates, performing diagnostic procedures, and assisting in anesthesia and surgery. While they may have the opportunity to cuddle the occasional puppy or kitten, a vet tech’s job is much more than playing with cute dogs and cats. -

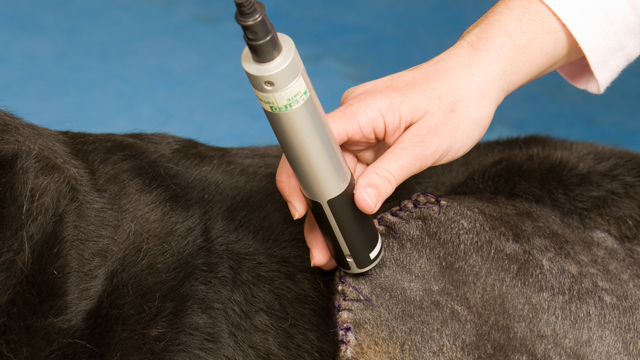
What is veterinary laser therapy?
What is veterinary laser therapy? Veterinary laser therapy is an innovative treatment that has gained popularity in recent years as veterinarians discover its benefits for pets. Used similarly to acupuncture, massage therapy, and other alternative therapies, laser treatment can be used in conjunction with, or instead of, medication to manage pain, inflammation, and wound healing. -

What should I know about my senior dog?
So, you just used the AAHA Canine Life Stage Calculator to determine that your dog is in the senior stage of life. Knowing your dog’s life stage helps you provide a lifetime of optimal care. -

What Common Household Items Are Toxic to Pets?
The American Society for the Prevention of Cruelty to Animals (ASPCA) Animal Poison Control Center (APCC) is a 24-hour helpline staffed by veterinary toxicologists and other veterinary professionals experienced in pet poisonings. Each year, the ASPCA APCC receives thousands of calls and compiles a list of the top 10 pet poisons, which most often are everyday household items. Here are the poisons currently topping the list and how you can keep your furry pal safe. -

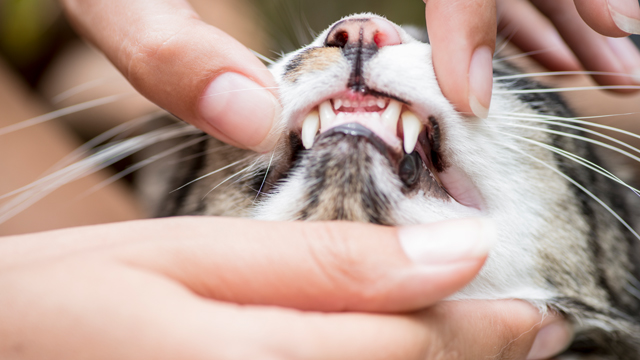
Do Pets Need Anesthesia for Dental Care?
You probably understand that routine dental care is crucial to your furry pal’s health, but did you know that anesthesia needs to be used during pet dental procedures? Anesthetizing your pet allows the veterinary team to perform a thorough oral health assessment, treat any dental issues they find, and prevent stress and discomfort for your pet. Although you may be concerned about anesthesia, your veterinarian takes specific precautions to minimize your pet’s risks and ensure their safety. -

What is limber tail in dogs?
Is anything sadder than your dog losing their wag? If your normally excitable pup fails to greet you with a whirling tail of excitement when you come home, that’s a sure sign something is wrong. The problem may be a condition called acute caudal myopathy, which goes by many other names, including: Limber tail Swimmer's tail Cold water tail Limp tail Rudder tail Broken wag Flaccid tail syndrome Sprained tail -

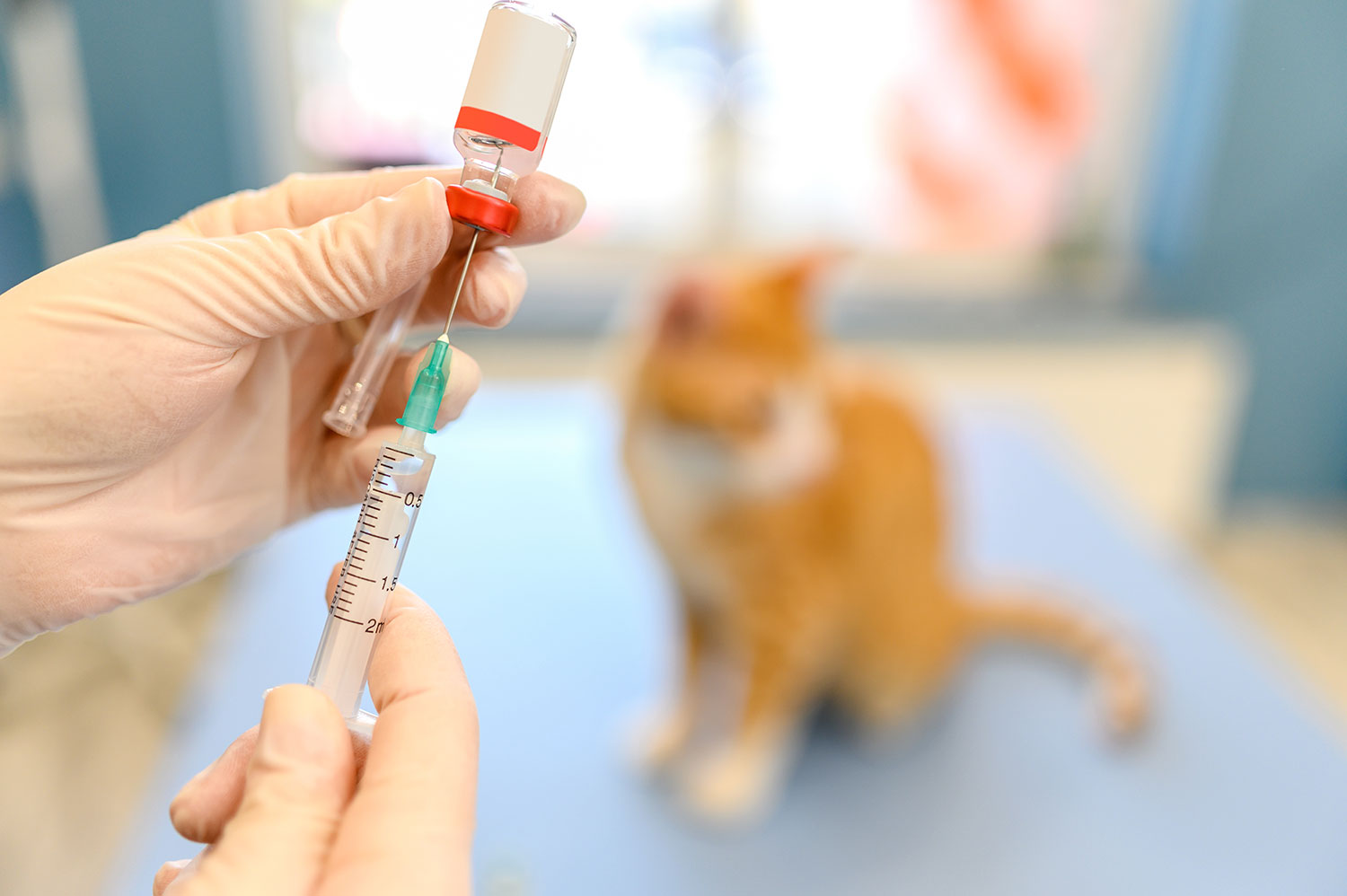
Should my pet be vaccinated?
Vaccination is a crucial and cost-effective method to protect your pet’s and the public’s health. Many diseases that affect our pets can spread via wildlife or unvaccinated pets, and several can also affect people. AAHA recommends all pets receive core vaccines—those deemed medically or legally necessary to meet minimum health standards—along with additional vaccines based on lifestyle. -

Can I volunteer with my pet?
Volunteering with your pet is a wonderful way to share the love and joy that animals bring people. Our canine and feline friends have talents and gifts to share, and nothing bonds people more closely than a furry companion. -

How can I tell if my pet has had a stroke?
Pet owners often don’t notice signs of a mild stroke in their companions since animals can’t say that they feel dizzy, can only see out of one eye, or are having memory problems. Unfortunately, pets usually experience strokes on a grander scale than people, and require immediate veterinary attention. -

How can I make my pet’s last day special?
Losing a loved one is never easy. Knowing your pet is nearing the end is bittersweet, because the grieving process often begins with a poor prognosis, but that also gives you time to create a special goodbye for your beloved companion. Celebrate a lifetime of love by treasuring your pet’s final moments and filling them with comfort and peace.